Abstract
Objective:
To assess the maternal sociodemographic, anthropometric, dietary and micronutrient status in apparently healthy pregnant women in order to determine their associations with intrauterine growth retardation (IUGR).
Design:
Prospective observational study.
Setting:
Bangalore City, India.
Subjects:
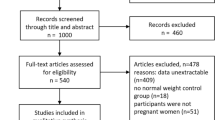
A total of 478 women were recruited at 12.9±3.3 weeks of gestation and followed up at the first, second and third trimesters of pregnancy and at delivery. The dropout rate was 8.5%.
Interventions:
None.
Main outcome measures:
Birth weight was measured at hospital delivery.
Results:
The mean birth weight was 2.85±0.45 kg. In all, 28.6% of newborns were IUGR. There was a strong inverse relationship between maternal educational level and risk of IUGR. A low body weight at baseline was also associated with a high risk of IUGR. Compared with women in the highest quartile for second trimester weight gain, those in the lowest quartile had a significantly higher adjusted odds ratio (AOR: 3.98; 95% CI: 1.83, 8.65) for IUGR. Women in the lowest tertile for serum vitamin B12 concentration during each of the three trimesters of pregnancy had significantly higher risk of IUGR (AOR: 5.98, 9.28 and 2.81 for trimesters 1–3, respectively).
Conclusions:
The present study demonstrates associations between educational status, maternal weight and gestational weight gain with IUGR. Importantly, in a subsample, there were strong associations of vitamin B12 status with IUGR, suggesting that better socioeconomic conditions, improved nutritional status and early detection of vitamin B12 deficiency in pregnancy combined with appropriate interventions are likely to play an important role in reducing IUGR.
Sponsorship:
This research was partly supported by the GlaxoSmithKline Consumer Healthcare Ltd, India.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Abrams B, Selvin S (1995). Maternal weight gain pattern and birth weight. Obstet Gynecol 86, 163–169.
ACC/SCN (1989). Malnutrition and infection. Tomkins A, Watson F (eds). ACC/SCN State-of-the-Art Series Nutrition Policy Discussion Paper No. 5. Administrative Committee on Coordination/Sub-Committee on Nutrition: Geneva.
ACC/SCN (2000). Low birthweight. Pojda J, Kelley L (eds). A Report Based on the International Low Birth Weight Symposium and Workshop Held in June 14–17, 1999, Dhaka, Bangladesh. Nutrition Policy Paper 18. Administrative Committee on Coordination/Sub-committee on Nutrition: Geneva.
Bui MH (1994). Simple determination of retinol, alpha-tocopherol and carotenoids (lutein, all-trans-lycopene, alpha- and beta-carotenes) in human plasma by isocratic liquid chromatography. J Chromatogr B Biomed Appl 654, 129–133.
de Onis M, Blossner M, Villar J (1998). Levels and patterns of intrauterine growth retardation in developing countries. Eur J Clin Nutr 52 (Suppl 1), S5–S15.
Dreyfuss ML, Msamanga GI, Spiegelman D, Hunter DJ, Urassa EJN, Hertzmark E et al. (2001). Determinants of low birth weight among HIV-infected pregnant women in Tanzania. Am J Clin Nutr 74, 814–826.
Durnin JVGA., Womersley J (1974). Estimates of total body fat from skinfold thickness: measurements on 481 men and women aged from 16 to 72 years. Br J Nutr 32, 77–79.
Fawzi WW, Msamanga GI, Spiegelman D, Urassa EJ, McGrath N, Mwakagile D et al. (1998). Randomised trial of effects of vitamin supplements on pregnancy outcomes and T cell counts in HIV-1-infected women in Tanzania. Lancet 351, 1477–1482.
Ferraz EM, Gray RH, Cunha TM (1990). Determinants of preterm delivery and intrauterine growth retardation in north-east Brazil. Int J Epidemiol 19, 101–108.
Fikree FF, Berendes HW (1994). Risk factors for intrauterine growth retardation: a community-based study in Karachi. Bull WHO 72, 581–587.
Finkelstein JD (1990). Methioine metabolism in mammals. J Nutr Biochem 1, 228–237.
Frery N, Huel G, Leroy M, Moreau T, Savard R, Blot P et al. (1992). Vitamin B12 among parturients and their newborns and its relationship with birthweight. Eur J Obstet Gynecol Reprod Biol 45, 155–163.
Gopalan C, Rama Sastri BV, Balasubramanian SC (1996). Nutritive value of Indian foods. Updated by Narasinga Rao BS, Deosthale YG, Pant KC. National Institute of Nutrition, Indian Council of Medical Research: Hyderabad.
Hibbard BM (1975). Folates and the fetus. S Afr Med J 49, 1223–1226.
Hickey CA, Cliver SP, McNeal SF, Hoffman HJ, Goldenberg RL (1996). Prenatal weight gain patterns and birth weight among nonobese black and white women. Obstet Gynecol 88, 490–496.
Kirke PN, Molloy AM, Daly LE, Burke H, Weir DG, Scott JM (1993). Maternal plasma folate and vitamin B12 are independent risk factors for neural tube defect. Q J Med 86, 703–708.
Kramer MS (2002). Balanced protein/energy supplementation in pregnancy (Cochrane review). In: The Cochrane Library Issue 4: CD 000032 Update Software: Oxford.
Mavalankar DV, Gray RH, Trivedi CR (1992). Risk factors for preterm and term low birth weight in Ahmedabad, India. Int J Epidemiol 21, 263–272.
Murphy MM, Scott JM, Arija V, Molloy AM, Fernandez-Ballart JD (2004). Maternal homocysteine before conception and throughout pregnancy predicts fetal homocysteine and birth weight. Clin Chem 50, 1406–1412.
O'Broin SD, Kelleher BP, Davoren A, Gunter EW (1997). Field study screening of blood folate concentrations: specimen stability and finger-stick sampling. Am J Clin Nutr 66, 1398–1405.
Osrin D, Vaidya A, Shrestha Y, Baniya RB, Manandhar DS, Adhikari RK et al. (2005). Effects of antenatal multiple micronutrient supplementation on birthweight and gestational duration in Nepal: double-blind, randomised controlled trial. Lancet 365, 955–962.
Rao S, Yajnik CS, Kanade A, Fall CH, Margetts BM, Jackson AA et al. (2001). Intake of micronutrient-rich foods in rural Indian mothers is associated with the size of their babies at birth: Pune Maternal Nutrition Study. J Nutr 131, 1217–1224.
Refsum H, Yajnik CS, Gadkari M, Schneede J, Vollset SE, Orning L et al. (2001). Hyperhomocysteinemia and elevated methylmalonic acid indicate a high prevalence of cobalamin deficiency in Asian Indians. Am J Clin Nutr 74, 233–241.
Roe JH, Kuether CA (1943). The determination of ascorbic acid in whole blood and urine through the 2,4-dinitrophenylhydrazine derivative of dehydroascorbic acid. J Biol Chem 147, 399–407.
Steegers-Theunissen RPM, Boers GHJ, Trijbels JMF, Eskes TKAB (1991). Neural-tube defects and derangement of homocysteine metabolism. N Engl J Med 324, 199–200.
Steegers-Theunissen RP, Boers GH, Blom HJ, Trijbels FJ, Eskes TK (1992). Hyperhomocysteinaemia and recurrent spontaneous abortion or abruptio placentae. Lancet 339, 1122–1123. (letter).
Steen MT, Bodie AM, Fisher AJ, MacMahon W, Saxe D, Sullivan KM et al. (1998). Neural-tube defects are associated with low concentrations of cobalamin (Vitamin B12) in amniotic fluid. Prenatal Diagn 18, 545–555.
Strauss RS, Dietz WH (1999). Low maternal weight gain in the second or third trimester increases the risk for intrauterine growth retardation. J Nutr 129, 988–993.
USDA Nutrient Data laboratory. (homepage) atwww.nal.usda.gov/fnic/foodcomp.
Vaz M, Bharathi AV, Muthayya S, Smitha J, Kurpad AV (in press). Food frequency questionnaire-based estimates of compliance to ATP III (national cholesterol education programme) recommended diets in a middle class adult population of Bangalore City. J Assoc Phys India.
Vollset SE, Refsum H, Irgens LM, Emblem BM, Tverdal A, Gjessing HK et al. (2000). Plasma total homocysteine, pregnancy complications, and adverse pregnancy outcomes: the Hordaland homocysteine study. Am J Clin Nutr 71, 962–968.
WHO (1995). Physical status: the use and interpretation of anthropometry. Report of a WHO expert committee. World Health Organ Tech Rep Ser 854, 1–452.
WHO (2001). Iron Deficiency Anaemia: Assessment, Prevention, and Control – A Guide for Programme Managers. World Health Organization: Geneva.
Zhou LM, Yang WW, Hua JZ, Deng CQ, Tao X, Stoltzfus RJ (1998). Relation of hemoglobin measured at different times in pregnancy to preterm birth and low birth weight in Shanghai, China. Am J Epidemiol 148, 998–1006.
Acknowledgements
We greatly appreciate the assistance of Nancy Nanditha, V Manjula, MN Selvi and Mercy in the collection and entry of data, and of JV Gnanou for sample handling and all laboratory measurements. We thank the women and their infants who participated in this study, and the doctors, nurses and laboratory technicians who made this study possible.
Author information
Authors and Affiliations
Corresponding author
Additional information
Guarantor: S Muthayya.
Contributors: SM was involved in study design and implementation, data analysis and writing of the manuscript. AVK was involved in study design, data analysis and writing of the manuscript. CPD, RJB and WWF provided expert advice on data analysis and write-up. PD was involved in study design, implementation and data entry. MV was involved in study design and write-up. AM, RM, AT and SB provided study subjects and facilities for this collaborative research. The authors have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Muthayya, S., Kurpad, A., Duggan, C. et al. Low maternal vitamin B12 status is associated with intrauterine growth retardation in urban South Indians. Eur J Clin Nutr 60, 791–801 (2006). https://doi.org/10.1038/sj.ejcn.1602383
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ejcn.1602383
Keywords
This article is cited by
-
Associations of prenatal metabolomics profiles with early childhood growth trajectories and obesity risk in African Americans: the CANDLE study
International Journal of Obesity (2021)
-
Placental expression of ENG, VEGF, and FLT: Gender-specific associations with maternal vitamin B12 status
European Journal of Clinical Nutrition (2020)
-
Type 1 Diabetes in a Resource-Poor Setting: Malnutrition Related, Malnutrition Modified, or Just Diabetes?
Current Diabetes Reports (2018)
-
Maternal B vitamins: effects on offspring weight and DNA methylation at genomically imprinted domains
Clinical Epigenetics (2016)
-
The association between maternal dietary micronutrient intake and neonatal anthropometry – secondary analysis from the ROLO study
Nutrition Journal (2015)