Abstract
Aims
Patients with diabetes mellitus experience a large number of falls and bone fractures that are not related solely to complications of the disease. The purpose of our study was to determine whether transient hyperglycemia affects attentional functions and gait.
Methods
This was a case–control study. We asked 17 patients with type 1 or type 2 diabetes mellitus to perform three visual tests and one visual and auditory attention test (Phasic Alert A1-4 and A2-3, Go/No Go, Intermodal Comparison). Mean response time (ms) and total number of errors were assessed. Ten of the patients also performed a tandem gait test consisting of three steps. The total distance travelled (TDT, in mm) by the center of pressure was measured with a pressure-sensitive calibrated platform. Transient hyperglycemia was defined as blood glucose level greater than 13, 8 mmol/L at the time of the test. These same patients were retested 1–3 days later at a blood glucose level at least 5, 5 mmol/L lower than the initial values (T24-72h). Nineteen patients with diabetes mellitus were matched with the original participants and performed the same test under normoglycemic conditions.
Results
During transient hyperglycemia, the mean response time (ms) and the TDT were significantly longer. The mean response time for the four tests increased by 53, 5 ms (P < 0.001). There was no increase in the number of errors. The TDT of the center of pressure increased significantly by 102 mm (P < 0.001).
Conclusions
Transient hyperglycemia alters attention and gait in patients with diabetes mellitus.

Similar content being viewed by others
References
Yamamoto M, Yamaguchi T, Yamaguchi M, Kaji H, Sugimoto T (2009) Diabetic patients have an increased risk of vertebral fractures independent of BMD or diabetic complications. J Bone Miner Res 24(4):702–709
De Liefde II, Van der Klift M, De Laet CE, Van Daele PL, Hofman A, Pols HA (2005) Bone mineral density and fracture risk in type 2 diabetes mellitus: the Rotterdam Study. Osteoporos Int 16(12):1713–1720
Schwartz AV, Sellmeyer DE, Ensrud KE, Cauley JA, Tabor HK, Schreiner PJ, Jamal SA, Black DM, Steven R Cunnings and for the study of osteoporotic fractures Research Group (2001) Older women with diabetes have an increased risk of fracture: a prospective study. J Clin Endocrinol Metab 86(1):32–38
Schwartz AV, Vittinghoff E, Bauer DC, Hillier TA, Strotmeyer ES, Ensrud KE, Donaldson MG, Cauley JA, Harris TB, Koster A, Womack CR, Palermo L, Black DM (2011) Association of BMD and FRAX score with risk of fracture in older adults with type 2 diabetes. JAMA 305(21):2184–2192
Melton LJ, Leibson CL, Achenbach SJ, Therneau TM, Khosla S (2008) Fracture risk in type 2 diabetes: update of a population-based study. J Bone Miner Res 23(8):1334–1342
Leslie WD, Rubin MR, Schwartz AV, Kanis JA (2012) Type 2 diabetes and bone. J Bone Min Res 27(11):2231–2237
Bianchi Lara et al (2016) Muscle dysfunction in type 2 diabetes: a major threat to patient’s mobility and independence. Acta Diabetol 53(6):879–889
Simó Rafael et al (2017) Cognitive impairment and dementia: a new emerging complication of type 2 diabetes—the diabetologist’s perspective. Acta Diabetol 54(5):417–424
McCrimmon, Ryan CM, Frier BM (2011) Diabetes and cognitive dysfunction. Lancet 16:2291–2299
Trento Marina et al (2015) Depression, anxiety and cognitive function in patients with type 2 diabetes: an 8-year prospective observational study. Acta Diabetol 52(6):1157–1166
Gonder-Frederick LA, Zrebiec JF, Bauchowitz AU, Ritterband LM, Magee JC, Cox DJ, Clarke WL (2009) Cognitive function is disrupted by both hypo- and hyperglycemia is school-aged children with type 1 diabetes: a field study. Diabetes Care 32:1001–1006
Rizzo MR, Marfella R, Barbieri M, Boccardi V, Vestini F, Lettieri B, Canonico S, Paolisso G (2010) Relationships between daily transient glucose fluctuations and cognitive performance among type 2 diabetic patients. Diabetes Care 33:2169–2174
Cox D, Kovatchev B, Gonder-Frederick L, Summers K (2005) Relationships between hyperglycemia and cognitive performance among adults with type 1 and type 2 diabetes. Diabetes Care 28:71–77
Pais I, Hallshmid M, Jauch-Chara K, Schmid SM, Oltmanno KM, Peeters A, Born J, Schultes B (2007) Mood and cognitive functions during transient euglycaemia and mild hyperglycemia in type 2 diabetes patients. Exp Clin Endocrinol Diabetes 115:42–46
Wessels AM, Sheltens P, Barkhof F, Heine RJ (2008) Hyperglycaemia as a determinant of cognitive decline in patients with type 1 diabetes. Eur J Pharmacol 585:88–96
Treisman AM, Gelade G (1980) A feature—integration theory of attention. Cogn Psychol 12:97–136
Renneboog B, Musch W, Vandermergel X, Manto MU, Decaux G (2006) Mild chronic hyponatremia is associated with falls, unsteadiness, and attention deficits. Am J Med 119:71e1-8
Zimmermann P, Fimm B (1995) Test for attentional performance (TAP). Psytest. http://www.psytest-fimm.com/Accessed. August 2012
De Wit B, De Clercq D, Aerts P (2000) Biomechanical analysis of the stance phase during barefoot and school running. Biomech 33:269–278
Praet SF, Louwerens JW (2003) The influence of shoe design on plantar pressure in neuropathic feet. Diabetes Care 26:441–445
Sommerfield A, Deary I, Frier B (2004) Transient hyperglycemia alters mood state and impairs cognitive performance in people with type 2 diabetes. Diabetes Care 27(10):2335–2340
Weinstein G, Maillard P, Himali J, Beiser A, Rhoda A, Wolf PA, Seshadri S, DeCarli C (2015) Glucose indices are associated with cognitive and structural brain measures in young adults. Neurology 84:2329–2337
Xia W, Wang S, Rao H, Spaeth AM, Wang P, Yang Y, Huang R, Cai R, Sun H (2015) Disrupted resting-state attentional networks in T2DM patients. Sci Rep 5:11148
Misawa S, Kuwabata S, Kanai K, Tamura N, Nakada M, Ogawara K, Yagui K, Hattori T (2006) Nodal currents in human diabetic nerves by the technique of latent addition. Clin Neurophysiol 117:815–820
Kikkawa Y, Kuwabara S, Misawa S, Tamura N, Kitano Y, Ogawara K, Hattori (2005) The transient effects of glycemic control on nerve conduction in human diabetics. Clin Neurophysiol 116:270–274
Saini AK, Arun HS, KauL L, Sharma S (2004) The transient effects of glycemic control nerve blood flow in male Sprague–Dawley: reversal by adenosin. Pharmacol Res 50:593–599
Teresa A, Hillier MD (1999) Hyponatremia: evaluating the correction factor for hyperglycemia. Am J Med 106:399–403
Vandergheynst F, Gombier Y, Bellante F, Perrota G, Remiche G, Mélot C, Mavroudakis N, Decaux G (2016) Impact of hyponatremia on nerve conduction and muscle strength. Eur J Clin Invest 46(4):328–333
Decaux G (2009) The syndrome of inappropriate secretion of antidiuretic hormone (SIADH). Semin Nephrol 29(3):239–256
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standard
The local ethics committee approved the study.
Informed consent
Written informed consent was obtained from each participant.
Additional information
Managed by Antonio Secchi.
Appendix
Appendix
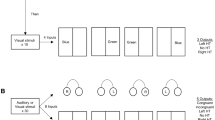
Description of the attentional tests. The tests included the following:
The subject was placed 50 cm from the screen of a laptop (the screen measured 32 cm diagonally) and kept his or her finger just above the validation key (button 1).
Go/No Go (25 trials)
The subject had to react quickly and selectively to one class of stimuli appearing successively on the screen (squares with different textures, only two of which are targets).
Intermodal Comparison (20 trials)
The subject was required to press a key as soon as there was a match between a pitch (high or low) and the direction of the arrow (up or down) that appeared on the screen.
Phasic Alert (20 trials preceded by an auditory warning: series 2–3; 20 trials not preceded by an auditory warning: series 1–4)
The subject must press a key as soon as a cross appears on the screen. In the second set of trials, the appearance of a cross was preceded by a beep.
Rights and permissions
About this article
Cite this article
Sattar, L., Renneboog, B. & Decaux, G. Hyperglycemia induces attention and gait deficits in diabetic mellitus patients. Acta Diabetol 54, 953–959 (2017). https://doi.org/10.1007/s00592-017-1034-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-017-1034-6